Decode Type 2 Diabetes Before It Spikes
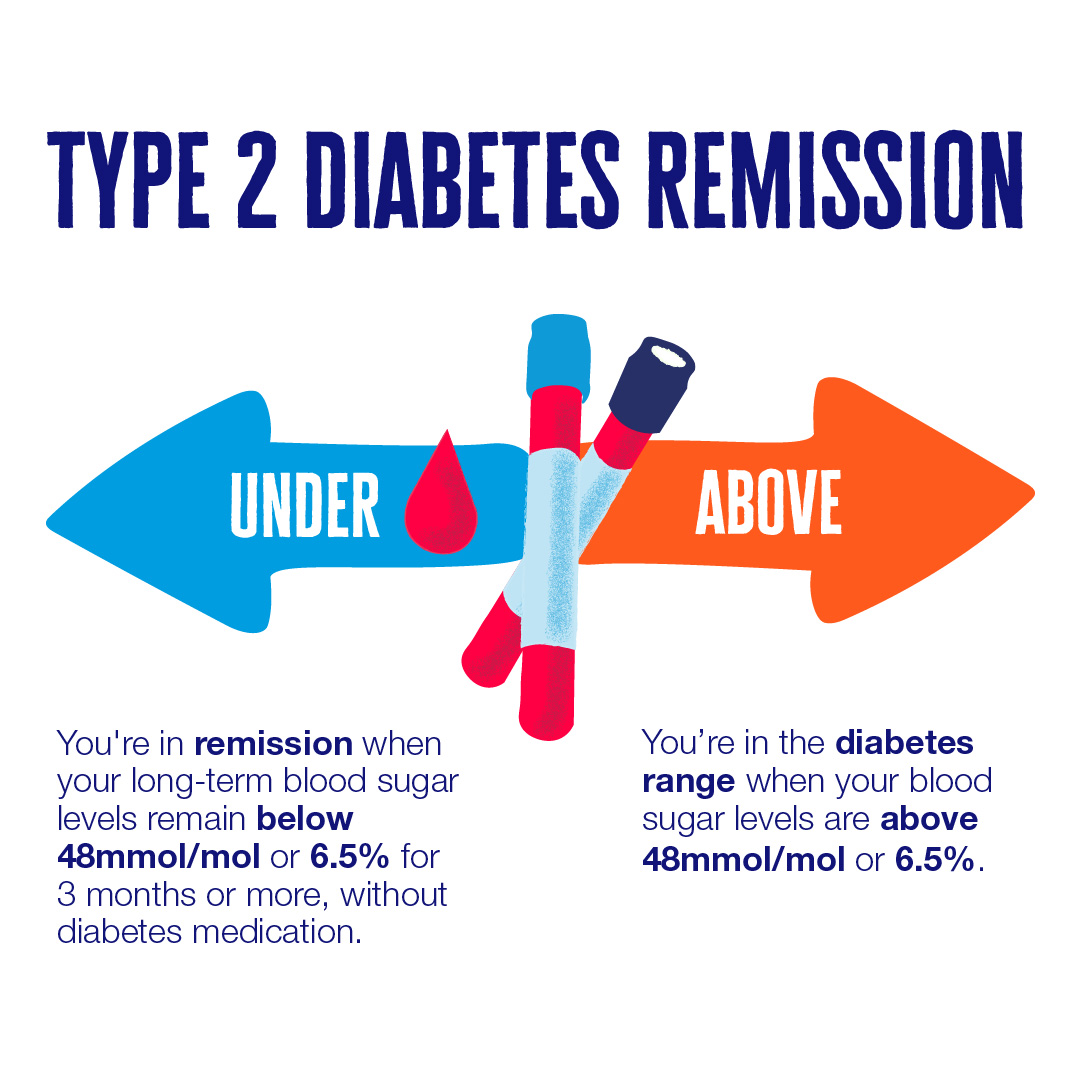
Type 2 diabetes reversal starts long before anyone sees a scary glucose chart. The real story begins years earlier with subtle metabolic drift: creeping insulin resistance, rising visceral fat, and silent inflammation. For anyone worried about energy crashes, stubborn weight, or a family history, recognizing these early signals is the difference between crisis care and a strategic comeback. The upside: these shifts are reversible with the right mix of muscle-first training, fiber-heavy meals, and consistent sleep. This guide unpacks how to spot the whispers before the shout and how to build a daily playbook that tilts metabolism back toward balance.
- Metabolic shifts show up years before a formal
type 2 diabetesdiagnosis. - Muscle mass and strength training protect glucose control better than cardio alone.
- Protein, fiber, and smart carbs flatten post-meal spikes and calm insulin demand.
- Sleep and stress shape hormones that govern appetite, cravings, and fat storage.
- Continuous monitoring beats annual labs for catching drift early.
Why Early Type 2 Diabetes Signals Matter
Most people assume type 2 diabetes reversal begins once HbA1c breaches the 6.5 percent line. In reality, the body has been negotiating insulin resistance for years. Muscle cells become less responsive to insulin, the liver leaks extra glucose, and fat cells release inflammatory signals that further blunt hormone sensitivity. Waiting for a lab flag means missing the easiest window for change. Catching drift early lets you fix mitochondrial efficiency, increase glucose uptake through movement, and reduce the pancreatic workload before beta cells burn out.
How to Spot the Quiet Metabolic Drift
Mainstream Labs You Should Not Ignore
Annual panels often include fasting glucose and triglycerides. Values that creep upward inside the “normal” range can still signal trouble. Pair them with HbA1c trends and ALT for fatty liver hints. If your waist-to-height ratio exceeds 0.5, assume visceral fat is rising.
Continuous Signals Beat Snapshots
Devices such as a continuous glucose monitor (CGM) reveal how meals, stress, and sleep shape glucose swings. Look for post-meal peaks above 140 mg/dL and time-in-range above 90 percent. Even without a CGM, a cheap glucometer plus a log of meals and workouts can expose patterns.
Energy and Cravings as Early Tells
Midday crashes, brain fog after refined carbs, or relentless evening snacking often point to insulin spikes followed by dips. These subjective cues can precede measurable lab drift, making them useful daily signals.
MainKeyword Playbook: Training for Type 2 Diabetes Reversal
Building and preserving muscle is the fastest lever for restoring insulin sensitivity. Muscle tissue stores and burns glycogen, acting as a glucose sink that eases the burden on the pancreas.
- Lift heavy 3-4 times per week focusing on compound moves:
squats,deadlifts,rows,presses. - Layer short cardio bouts post-meal: a 10-minute walk after eating blunts spikes.
- Use
high-intensity interval training1-2 times weekly to enhance mitochondrial efficiency. - Track progress with strength milestones and body composition, not just the scale.
“Muscle is a metabolic currency – the more you have, the easier it is to keep glucose in range.”
Sample Weekly Protocol
Mon: Push day + 10-minute post-dinner walkTue: 20-minute intervals on a bikeWed: Pull day + core stabilityThu: Mobility + brisk 30-minute walkFri: Lower body + post-meal walkSat: Light hike or swimSun: Rest, stretch, early bedtime
Nutrition That Calms Insulin
The goal is to reduce glucose volatility, not eliminate carbs. Pairing carbs with protein and fat slows absorption, while fiber reduces peak height.
- Prioritize 25-35g protein per meal from
eggs,fish,lentils, orGreek yogurt. - Hit 30-40g daily fiber via
beans,berries,chia seeds, and leafy greens. - Swap refined grains for whole sources like
steel-cut oatsandquinoa. - Use vinegar or citrus before carb-heavy meals to moderate glucose response.
- Time carbs after training sessions when muscles are primed to uptake glucose.
Code-Like Meal Template
Plate = 1/2 colorful veg + 1/4 lean protein + 1/4 slow carb + 1 thumb healthy fat
This simple heuristic keeps macronutrient balance front and center without calorie counting.
Sleep and Stress: The Hidden Hormonal Switches
One bad night can drop insulin sensitivity by double digits. Chronic stress elevates cortisol, which raises fasting glucose and fuels belly fat.
- Set a fixed lights-out time to secure 7-9 hours. Treat it like a non-negotiable meeting.
- Use
morning lightexposure to anchor circadian rhythms and improve sleep drive. - Practice 5-minute
box breathingsessions before meals to slow cortisol spikes. - Limit evening screens; blue light delays
melatoninand worsens sleep quality.
“Sleep debt is metabolic debt. You cannot out-lift or out-diet a broken circadian rhythm.”
Monitoring and Metrics That Matter
Data closes the feedback loop, revealing which habits move the needle.
Time-in-rangefrom a CGM: Aim for 90 percent between 70-140 mg/dL.Resting heart rate: Lower numbers suggest better recovery and metabolic health.Waist circumference: Track monthly; shrinking inches often precede weight changes.Strength PRs: Rising numbers mean more muscle mass and better glucose disposal.
DIY Metrics Pipeline
Collect: Morning weight, waist, fasting glucoseTag: Meals, workouts, sleep hoursReview: Weekly trends, not daily noiseAdjust: Move carbs toward training days, add walks after higher-carb meals
Why This Matters for the Next Decade
Demographics and food environments make type 2 diabetes the defining metabolic threat of this era. Yet the same levers that reverse early drift – muscle, fiber, sleep, stress control – also cut cardiovascular risk, sharpen cognition, and extend healthspan. The preventive window is wide open, but it rewards those who act before a diagnosis. Treat these habits as infrastructure: build them now so that in five years your lab numbers, energy, and mood all point in the same direction.
Actionable Roadmap in 30 Days
Week 1: Audit current habits. Get baseline HbA1c, fasting glucose, waist, and resting heart rate. Start post-meal walks.
Week 2: Add two strength sessions and increase protein to 1.6g/kg body weight.
Week 3: Layer fiber to 30g daily and swap refined carbs for slow carbs.
Week 4: Lock in sleep schedule and test a CGM or glucometer-driven meal experiment.
Small changes compound. By the end of a month, expect steadier energy, flatter glucose curves, and better training output. Keep iterating: the goal is not perfection but a metabolic environment where glucose management is boringly consistent.
The information provided in this article is for general informational purposes only. While we strive for accuracy, we make no guarantees about the completeness or reliability of the content. Always verify important information through official or multiple sources before making decisions.