Hantavirus Cases Rise as CDC Sounds Alarm
Hantavirus is the kind of threat that thrives in the blind spot between public memory and public health readiness. It is rare, often misunderstood, and brutally serious when it strikes. That combination is exactly why new CDC concern around hantavirus cases in Americans matters more than the numbers alone might suggest. When a disease carries a high fatality risk, even a relatively small cluster can expose larger weaknesses in awareness, diagnosis, and prevention. For readers trying to separate panic from genuine risk, the real question is not whether hantavirus is suddenly everywhere. It is whether health systems and households are prepared to recognize the warning signs before a preventable exposure becomes a medical emergency.
- Hantavirus remains rare, but it can become life-threatening fast.
- The biggest risk often comes from exposure to infected rodent droppings, urine, or saliva in enclosed spaces.
- CDC attention signals a need for sharper public awareness, not automatic panic.
- Early symptoms can look like common viral illness, which makes delayed diagnosis a real danger.
- Prevention depends on safe cleanup practices, rodent control, and understanding where exposure happens.
Why the hantavirus warning hits differently now
The latest attention on hantavirus lands at a moment when Americans are already recalibrating how they think about infectious disease. The pandemic era trained the public to watch dashboards and headlines, but it also created a new problem: alert fatigue. That is why a CDC warning about a less common pathogen can be easy to shrug off.
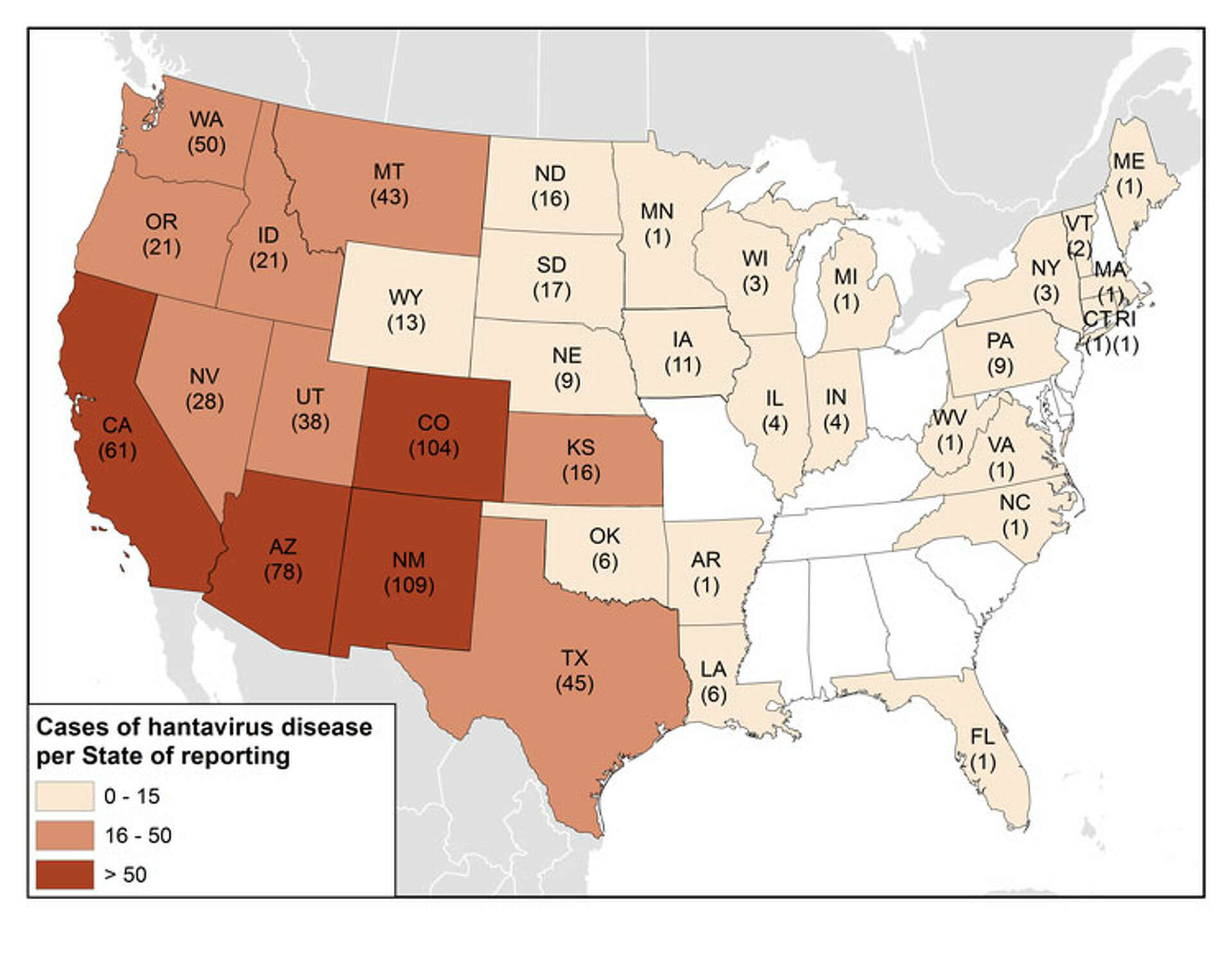
That would be a mistake. Hantavirus does not behave like a routine seasonal bug. In the United States, infections are often linked to contact with infected rodents, especially deer mice, and exposure can happen while cleaning cabins, sheds, garages, crawl spaces, or other areas where droppings have accumulated. The threat is not simply being near a mouse. It is the inhalation of contaminated particles that become airborne when people sweep, vacuum, or disturb dried waste.
Rare does not mean trivial. In public health, a low case count paired with a high severity profile deserves more attention than many people give it.
That is the strategic tension here. Hantavirus is not a mass-transmission event in the way influenza or respiratory viruses can be. But when it appears, it tends to arrive with unusually high stakes.
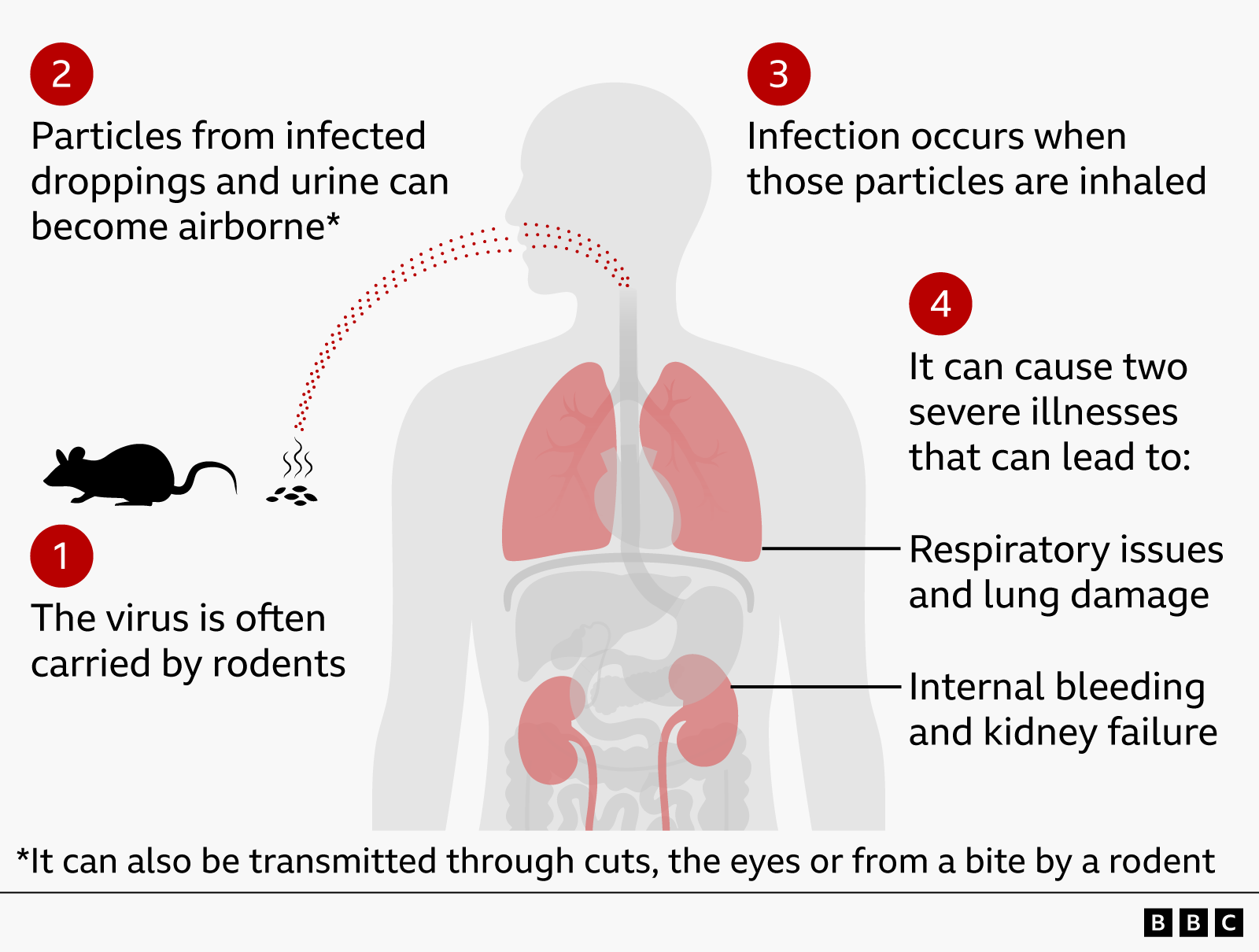
How hantavirus infection happens
Understanding hantavirus starts with the transmission pathway. In the U.S., the virus is primarily associated with rodents carrying the pathogen without appearing sick themselves. Humans can become infected after breathing in virus particles from contaminated nesting material or waste. Less commonly, transmission may also occur through touching contaminated surfaces and then touching the nose or mouth, or through rodent bites.
This matters because the most dangerous exposures often occur during ordinary chores. Opening an old vacation home for the season. Clearing a shed after winter. Cleaning a basement corner that has gone untouched for months. These are not exotic scenarios. They are exactly the kinds of moments when people move fast, skip protective steps, and unknowingly create the conditions for infection.
High-risk environments to watch
- Closed-up cabins or seasonal homes with visible rodent activity
- Sheds, barns, garages, and attics where droppings may have dried out
- Crawl spaces and storage rooms with nesting material
- Rural or semi-rural properties where rodents can enter easily
- Cleanup after long periods of vacancy when contamination has built up unnoticed
The hard part is that these settings can feel harmless right up until they are not. Hantavirus often exploits the exact gap between familiarity and caution.
Why diagnosis is so difficult
One reason hantavirus remains especially dangerous is that early symptoms can resemble a broad range of common illnesses. Fever, fatigue, muscle aches, headache, nausea, and abdominal discomfort do not immediately scream rare rodent-borne virus. They can look like flu, food poisoning, or a generic viral infection.
That diagnostic ambiguity creates a race against time. In some patients, the illness can escalate into severe respiratory distress, sometimes progressing rapidly enough to require intensive care. By the time breathing problems become obvious, the window for early intervention may already be narrowing.
Symptoms that should change the conversation fast
If a patient develops a flu-like illness after recent exposure to rodent-infested spaces, that context is not a footnote. It is central. Clinicians and patients alike need to connect environmental exposure with symptoms as early as possible.
- Fever and deep fatigue
- Muscle pain, especially in large muscle groups
- Nausea, vomiting, or abdominal pain
- Dizziness or chills
- Shortness of breath or worsening respiratory symptoms
The biggest practical takeaway is simple: if symptoms follow recent rodent exposure, say so immediately. That kind of detail can shape testing, monitoring, and treatment decisions.
What the CDC concern really signals
A federal health warning does not always mean a disease is exploding across the country. Often, it means something more precise and more important: awareness is lagging behind risk. In the case of hantavirus, that gap can be deadly.
Public health agencies issue alerts to sharpen recognition, especially when severe disease may be underappreciated or when recent cases suggest a pattern worth amplifying. The strategic goal is not to trigger broad fear. It is to improve prevention and reduce delays in diagnosis.
The CDC message is less about scale than consequence. A disease does not need millions of cases to justify urgent communication if the outcomes are severe enough.
That distinction matters for news consumers. The modern information ecosystem tends to flatten every health alert into one of two bins: overblown or catastrophic. Hantavirus sits in neither. It is a targeted but serious threat, one that demands practical caution from specific populations and regions rather than universal alarm.
How to reduce hantavirus risk at home
The best defense against hantavirus is not a pharmaceutical breakthrough. It is disciplined environmental hygiene and safer cleanup behavior. This is where public health advice can sound almost too basic, but basic does not mean optional.
Safer cleanup steps that actually matter
- Do not sweep or vacuum dry droppings. That can aerosolize infectious particles.
- Ventilate closed spaces first. Open doors and windows before entering and cleaning.
- Use disinfectant or a bleach solution. Wet contaminated areas thoroughly before wiping them up.
- Wear gloves. In higher-risk situations, added respiratory protection may also be appropriate.
- Seal entry points. Rodent-proofing is prevention, not cosmetic maintenance.
For households, the tactical mindset should be clear: treat rodent evidence as a health issue, not just a nuisance. If you are dealing with heavy infestation, a casual cleanup with a broom and no protection is the wrong move.
Pro tip for property owners
Seasonal properties deserve a pre-entry checklist. Before the first major cleanup, inspect for droppings, nesting, gnaw marks, and food contamination. A slow, ventilated, wet-clean approach is smarter than a quick reset.
Even simple routines can help. Think in terms of contamination control rather than tidiness. The goal is to avoid turning a hidden problem into an airborne one.
Why this matters beyond one disease
The larger significance of the hantavirus story is not just about one pathogen. It is about how public health handles low-frequency, high-severity risk. These are the threats that often struggle for attention because they do not fit mass-media instincts. They are too rare for everyday coverage and too serious to ignore.
That creates a policy challenge. Health systems are generally built to respond to volume, but some of the most consequential interventions involve awareness rather than scale. A rural physician recognizing a possible hantavirus case earlier. A family cleaning a cabin correctly. A local health department circulating practical guidance before summer travel and property reopening begin. Those actions do not make splashy headlines, but they save lives.
There is also an equity angle. People in rural communities, agricultural settings, or older housing stock may face higher exposure risk, while also having less immediate access to specialty care. That is exactly where clear communication and faster recognition become most valuable.
What to watch next
The near-term question is whether public attention translates into behavior change. If CDC concern leads more clinicians to ask about rodent exposure and more households to rethink cleanup practices, the impact could be meaningful even without large case numbers.
Longer term, expect more emphasis on environmental health intelligence: regional rodent patterns, seasonal behavior, housing conditions, and targeted risk communication. This is not a technology-first story. It is a preparedness story. And preparedness, in public health, usually looks less like dramatic intervention and more like a thousand small decisions made correctly.
For readers, the practical conclusion is refreshingly concrete. Know where hantavirus risk comes from. Take rodent signs seriously. Clean contaminated spaces the right way. And if illness follows exposure, make that history impossible for a clinician to miss.
That may not feel revolutionary. But when the disease in question can move from vague symptoms to respiratory crisis with unnerving speed, ordinary caution becomes a powerful form of prevention.
The information provided in this article is for general informational purposes only. While we strive for accuracy, we make no guarantees about the completeness or reliability of the content. Always verify important information through official or multiple sources before making decisions.