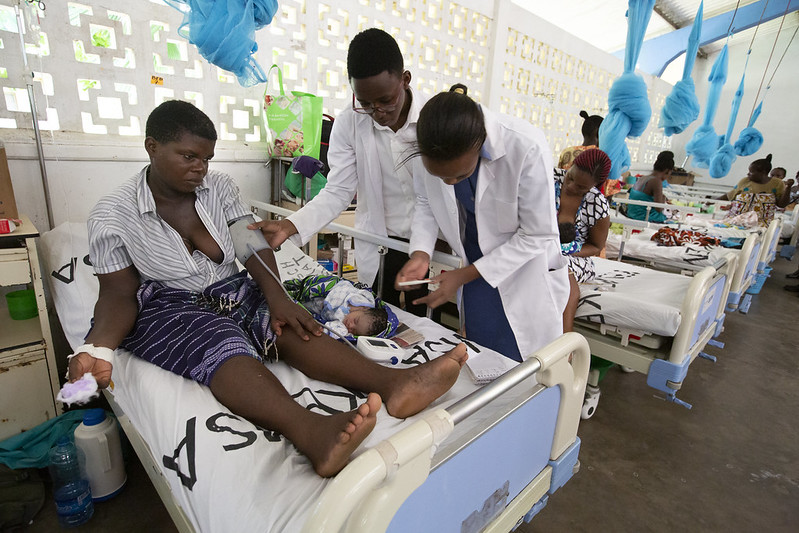
Hantavirus Outbreak Shakes Cruise Travel
Hantavirus Outbreak Shakes Cruise Travel
Travel operators sell control: controlled routes, controlled dining, controlled comfort. Infectious disease keeps proving otherwise. A hantavirus outbreak linked to a cruise-associated journey is the kind of public health scare that instantly rattles passengers and forces health officials into a high-speed investigation. The concern is not just that hantavirus is rare. It is that rare pathogens are uniquely disruptive because they sit outside the average traveler’s mental checklist. People know to think about norovirus on ships. Far fewer think about rodent-borne viruses connected to lodging, excursions, or supply environments during a trip. That gap matters. When an unusual illness appears in a travel setting, the response has to move fast, communicate clearly, and avoid both panic and complacency.
- Hantavirus is rare but serious, and even a small cluster can trigger a major health response.
- The cruise angle matters because travel creates complex exposure chains across ships, hotels, transport, and shore stops.
- Public health investigators must trace environments, not just people, since
hantavirusoften spreads through exposure to infected rodent waste. - For travelers and operators, trust is the real battleground: slow or vague communication can do lasting damage.
Why the hantavirus outbreak feels bigger than the case count
Not every outbreak becomes a headline. A hantavirus outbreak does because it hits three pressure points at once: severity, uncertainty, and unfamiliarity. Unlike common cruise illnesses that spread person to person in obvious ways, hantavirus usually enters the picture through inhalation of virus particles from rodent urine, droppings, or saliva that have become airborne. That immediately widens the investigation. Officials are no longer asking only who sat near whom or who ate what. They are asking where travelers slept, what enclosed spaces they entered, how supplies were handled, and whether any buildings or vehicles had signs of rodent activity.
That complexity is what makes the story important beyond one itinerary. Modern travel is a chain of environments. A passenger may fly, board a bus, stay in a lodge, take excursions, and embark on a ship – all within days. A serious infection tied to any one link can appear, at first glance, to be a cruise outbreak even if the most likely exposure happened elsewhere.
Rare diseases do not need huge numbers to create huge consequences. They just need enough uncertainty to expose weak spots in detection, communication, and environmental safety.
What hantavirus actually is
Hantavirus is not one single disease label people use casually, and that is part of the communication problem. In the United States, public health discussions often focus on infections that can lead to hantavirus pulmonary syndrome, a severe respiratory illness that can begin with symptoms that look deceptively ordinary: fever, fatigue, muscle aches, headache, and sometimes nausea or abdominal symptoms. As the disease progresses, breathing can become difficult and the situation can turn critical fast.
The main transmission route is environmental exposure to contaminated rodent waste, especially in enclosed areas where viral particles can be stirred into the air. That means cabins, storage areas, outbuildings, lodges, utility rooms, or rarely used spaces become important points of review. It also means many travelers may not realize they were in a risk setting at all.
Why early symptoms are a problem
Early illness can look like flu, COVID-19, or another viral infection. For clinicians, that creates a difficult window. If a patient presents after travel with fever and body aches, a rare rodent-borne infection is not always the first assumption. That makes public health alerts especially valuable. Once doctors know a patient was part of a trip under investigation, the threshold for considering hantavirus changes.
Why cruise-associated cases draw extra scrutiny
Cruises are highly visible brands operating in a heavily regulated environment. Any mention of an outbreak immediately raises questions about sanitation, disclosure, and duty of care. Even when the ship itself may not be the root cause, the operator can still face the reputational blast radius because the cruise package is what binds the traveler experience together in the public mind.
How investigators likely approach a cruise-linked hantavirus outbreak
This is where outbreak response becomes less cinematic and more methodical. Public health teams are typically trying to solve two problems at the same time: identify who was exposed and identify where the exposure happened. Those are different tasks.
1. Build a timeline
Investigators reconstruct the itinerary in granular detail. That includes embarkation, lodging before or after boarding, transportation links, shore excursions, and any shared facilities. A timeline can reveal whether ill travelers overlapped in a specific place for a specific duration.
2. Separate shipboard spread from environmental exposure
This distinction matters. A disease like norovirus can race through passengers by direct contamination and close contact. Hantavirus points attention instead toward environmental contamination involving rodents. If cases cluster among people who visited the same lodge, storage space, scenic stop, or transport hub, that may become the focal point rather than the vessel itself.
3. Look for rodent evidence
Environmental inspections often involve signs such as droppings, nesting material, gnaw marks, food contamination, and poorly sealed structures. Ventilation and cleaning practices may also come under review. One critical public health point: sweeping or vacuuming contaminated droppings can aerosolize viral particles, which is why cleanup guidance matters.
4. Alert clinicians and travelers
Because symptoms may not appear immediately, outreach is essential. Exposed travelers need clear information on what symptoms to watch for and when to seek care. Medical providers need notice so they can ask the right travel-history questions and escalate testing or treatment decisions appropriately.
Why this matters for the travel industry
The travel business has spent years rebuilding confidence after pandemic-era disruption. A hantavirus outbreak does not threaten travel in the same way a highly transmissible respiratory virus does, but it stresses a different part of the system: credibility. Passengers want to know that operators understand risks beyond the usual checklist and can communicate precisely when something unusual happens.
That is harder than it sounds. Overreaction can cause unnecessary panic. Underreaction can look evasive. The companies that handle these moments best tend to do three things well: they acknowledge what is known, clearly label what is not yet known, and explain what actions are underway.
When an outbreak is unusual, transparency becomes part of the health response, not just the public relations response.
Operational lessons cruise companies should take seriously
- Environmental risk audits cannot stop at the ship. Partner lodges, transport providers, excursion operators, and storage facilities all matter.
- Rodent control is a systems issue. It depends on food storage, waste handling, maintenance, sealing access points, and inspection frequency.
- Health messaging should be pathogen-specific. A generic advisory is less useful than one that explains how
hantavirusexposure differs from common onboard illnesses. - Staff training matters. Crew and travel coordinators should know how to escalate reports involving unusual symptoms or environmental concerns.
What travelers should actually do
Most passengers will never encounter a trip touched by hantavirus. But rare does not mean irrelevant. The smarter takeaway is not fear. It is situational awareness.
Pro tips for travelers
- If a travel provider sends a post-trip health notice, read it fully rather than assuming it is routine legal language.
- After travel, seek medical care promptly for fever, severe muscle aches, or breathing symptoms, especially if public health authorities mention possible exposure.
- Pay attention to environmental red flags during travel: rodent sightings, droppings, musty enclosed spaces, or visibly poor maintenance in cabins or lodges.
- Avoid disturbing rodent waste. Do not sweep or vacuum suspicious droppings in enclosed spaces.
The practical lesson here is simple: if your itinerary included an area under investigation, your travel history becomes medically relevant. Tell clinicians where you went, when you went, and whether you received any exposure notification. That information can materially change the clinical decision-making process.
The bigger shift in outbreak detection
One reason stories like this now travel faster is that surveillance has changed. Public health teams, travel operators, and clinicians are better connected than they were years ago. Passenger manifests, symptom reports, and coordinated alerts can help identify clusters earlier. That does not eliminate risk, but it compresses the time between a strange illness and a focused response.
There is also a broader expectation shift. Travelers increasingly assume that companies can trace, notify, and explain. In many cases they can – but only if records are good, local partners are cooperative, and communication lines are not fragmented across jurisdictions. A cruise-linked investigation can cross cities, states, or even countries. That makes standardization incredibly important.
Where systems still break down
Rare disease events often reveal the rough edges of coordination. Terminology may vary. Exposure windows may be revised. Initial reports may overemphasize the most visible part of the trip rather than the most plausible source of exposure. None of that necessarily means officials are failing. It often means they are working through uncertainty in public view.
Still, the lesson for organizations is clear: crisis planning should include low-probability, high-impact scenarios. If the only outbreak playbook is built around norovirus or flu-like spread, teams may be slow to handle a rodent-borne threat that requires environmental investigation and more nuanced messaging.
What happens next after a hantavirus outbreak alert
After the first wave of concern, the response usually enters a quieter but more consequential phase. Investigators refine case definitions, rule out unrelated illnesses, inspect suspect environments, and issue targeted follow-up guidance. The public may lose interest before the operational lessons are fully absorbed. That would be a mistake.
The real test is whether operators and public health agencies turn a rare incident into durable prevention. That can mean tighter inspection protocols, stronger partner oversight, better cleaning procedures for rodent contamination, and clearer traveler communications. It can also mean designing incident-response templates that are flexible enough to address uncommon pathogens without sounding generic or confusing.
The bottom line: this hantavirus outbreak is a reminder that modern travel risk is not limited to the obvious pathogens people associate with ships, airports, or crowds. Sometimes the biggest threat sits in the background – environmental, uncommon, and easy to miss until someone gets very sick. That is exactly why the response has to be sharper than the headlines.
The information provided in this article is for general informational purposes only. While we strive for accuracy, we make no guarantees about the completeness or reliability of the content. Always verify important information through official or multiple sources before making decisions.